1. Introduction: The Silent Science of the Food Bowl
In today’s pet “wellness” culture, the noise is deafening. Between the grain-free debates echoing across social media and the artisanal toppers trending at the local boutique, owners are under immense pressure to obsess over brand names and ingredient lists. Yet, while we audit the marketing on the bag, we often overlook the metabolic landscape where health is actually won or lost.
Recent clinical insights from the 2021 and 2023 AAHA guidelines have revealed that much of what we consider “common sense” in pet care is actually counter-intuitive. To truly advocate for our companions, we must move past the food-bowl theater and understand the clinical pillars that dictate animal longevity.
2. Nutrition is the “Fifth Vital Assessment”
For decades, nutrition was treated as a secondary lifestyle factor—a choice akin to picking a collar color.
The science has shifted. Nutrition is now formally recognized as the “fifth vital assessment.”
This puts it on the same clinical plane as temperature, pulse, respiration, and pain.
It is no longer an “extra” for overweight pets. It is a foundational pillar of every single veterinary visit.
Whether your pet is there for a routine vaccine or a broken nail, a nutritional audit must occur.
This systematic evaluation ensures that diet-specific safety, feeding environment, and human factors are within a safe metabolic threshold.
“Nutritional management is a central component of a complete healthcare plan for canine and feline patients and is integral to a pet’s longevity and quality of life.”
3. The “Muscle vs. Fat” Paradox: Why BCS Isn’t Enough
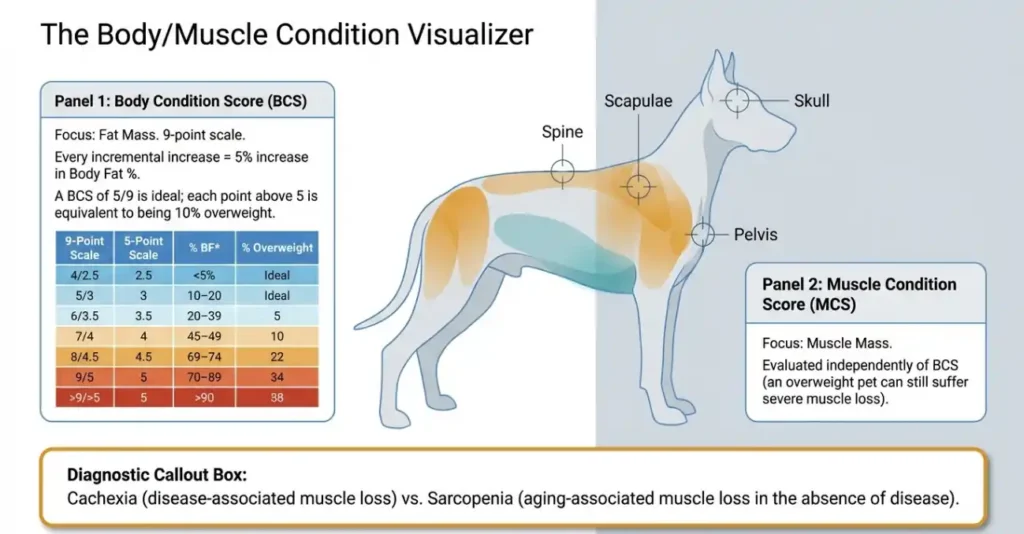
Most sophisticated owners are familiar with the Body Condition Score (BCS)—the 9-point scale used to assess body fat. However, evaluating fat is only half the battle. To gain a true “pro” perspective on health, we must separate BCS from the Muscle Condition Score (MCS).
The paradox is that an animal can be overweight (a high BCS) while simultaneously suffering from significant muscle loss. Whether it is sarcopenia (aging-related) or cachexia (disease-related), muscle wasting is a critical prognostic indicator of mortality. It doesn’t just look bad; it adversely affects clinical outcomes and longevity.
Because fat can mask the decline of lean body mass, you must look beyond the “number on the scale.” A professional assessment requires manual palpation of the spine, scapulae (shoulder blades), skull, and pelvis. If you can feel bone through these areas, your pet may be “fat and wasting” simultaneously—a high-risk state that requires immediate intervention.
“BCS and MCS are not causally related and should be assessed separately.”
4. The 10% Rule: The Hidden Math of Treats
We often use food as a language of love, but this emotional anthropomorphism can push a pet past a dangerous metabolic threshold. The “10% rule” is a strict clinical requirement: any item that is not “complete and balanced”—including toppers, dental chews, and table scraps—must not exceed 10% of a pet’s total daily calories.
When this limit is breached, it creates a “double-edged sword”: the pet suffers from excess calories leading to obesity, while simultaneously experiencing “nutrient dilution.” Essentially, the treats crowd out the essential vitamins and minerals in the primary diet, leading to a state of being both overfed and malnourished.
To manage this, view weight management as precision medicine. Traditional measuring cups are a liability; they are notoriously inaccurate and a primary driver of the pet obesity epidemic. For true precision, swap the cup for a gram scale.
Hidden Calorie Sources (The Audit List):
- Medication Vehicles: Peanut butter, cheese, or meat used to hide pills.
- Dental Chews: Often perceived as “health items” but frequently high in caloric density.
- Artisanal Toppers: Extra scoops of “human-grade” chicken or wet food added to dry kibble.
- Training Rewards: High-frequency, small treats that rapidly accumulate during a single session.
5. The “Natural” Supplement Trap
The irony of the modern holistic movement is that “natural” is often conflated with “safe.” In reality, mixing supplements with prescription medications can create a toxic landscape within the liver, stomach, and intestines.
Certain drugs can inhibit the very enzymes responsible for metabolizing supplements, leading to a dangerous build-up in the pet’s system. For example, Echinacea—a staple for immune support—can significantly alter the efficacy of chemotherapy drugs.
For the sophisticated consumer, transparency is key. While many human supplements are found to contain hidden drugs or contaminants, animal-specific products carrying the NASC (National Animal Supplement Council) seal are held to a higher standard of transparency, requiring rigorous certificates of analysis for each batch.
“Drugs can alter the potency of herbs and supplements, can cause side effects.”
6. The Insurance Paradox: It’s Not Just About the Bill
Pet insurance is rarely a simple financial calculation; it is an ethical one. To understand its value, we must look at the Veterinary Client Hierarchy of Needs. Before we can reach “Partnership” and “Communication,” a pet’s basic “Safety and Physiological” needs must be met.
There is a sharp distinction between an owner’s willingness to pay (fueled by the human-animal bond) and their dispensable funds (the reality of the wallet). Insurance acts as a bridge, removing the “price tag” from the exam room and allowing the veterinarian and owner to focus exclusively on the animal’s welfare.
The data is clear: insured dog owners spend 29% more on care, and cat owners spend 81% more. This isn’t just because they have more money; it’s because insurance provides “risk equalization,” mitigating financial spikes and freeing owners to consider only the best clinical path. While it may not solve the crisis for those with truly limited resources, it transforms the care relationship for those who use it.
7. Conclusion: The Future of the “Senior” Years
As we lean into the 2023 Senior Care philosophy, we must internalize a singular truth: “Old age is not a disease.” The senior years are a distinct life stage that requires a proactive, tailored healthcare plan—not a period of expected, unmanaged decline.
By auditing your pet’s nutritional landscape, prioritizing muscle mass over scale weight, and choosing supplements with clinical transparency, you aren’t just feeding a pet; you are engineering longevity.
If nutrition is the fifth vital sign, are you listening to what your pet’s body is trying to tell you—or just what’s on the label of the bag?

|
Topic of Concern
|
Animal Life Stage/Condition
|
Nutrients of Concern
|
Clinical Assessment/Diagnostic Methods
|
Management & Communication Strategies
|
Insurance & Financial Considerations (Inferred)
|
Source
|
|---|---|---|---|---|---|---|
|
Nutritional Assessment & Lifecycle Management
|
All Life Stages
|
Essential nutrients (complete and balanced), caloric intake (/ calculation)
|
9-point Body Condition Score (BCS), Muscle Condition Score (MCS), Diet History Form (DHF), Body Fat Index (BFI), Girth assessment, Fecal scoring
|
Universal use of 9-point scale; teach owners to assess BCS/MCS; nonjudgmental communication; use of food-dispensing toys; clear nutrition recommendations (7x more likely to adhere)
|
Routine wellness panels and diagnostic screenings are often covered by pet insurance wellness add-ons, reducing out-of-pocket costs for regular assessments.
|
[1]
|
|
Chronic Kidney Disease (CKD)
|
Senior / Geriatric Cats and Dogs
|
Low phosphorus, potassium supplementation, high EPA/DHA, increased energy density (to maintain LBM), restrictive protein (IRIS Stage 3)
|
SDMA assay, Creatinine, USG, UP:UC ratio, Blood pressure monitoring
|
Caution with senior diets (may have high phosphorus); use of phosphate binders; maintaining hydration through daily fluid therapy
|
Pet insurance covering chronic conditions (like Figo or Pets Best) can offset the high cost of specialized therapeutic diets and regular laboratory monitoring.
|
[1], [2], [3]
|
|
Cardiovascular Disease
|
Senior Dogs and Cats
|
Controlled sodium, high EPA/DHA, taurine (DCM), L-carnitine, avoid low protein (HCM)
|
NT-proBNP, Echocardiogram, Thoracic radiographs, Electrocardiogram (ECG), Blood pressure
|
Avoid grain-free or legume-heavy diets in dogs (DCM risk); owner education on sleeping respiratory rate
|
Advanced diagnostics like echocardiograms are expensive; specialized emergency coverage (like Spot) helps manage costs of congestive heart failure crises.
|
[1], [2], [3]
|
|
Osteoarthritis
|
Senior / Obese Pets
|
High EPA/DHA, Glucosamine, Chondroitin, added Antioxidants, low energy density (for weight control)
|
Chronic pain scales, limb girth assessment, orthopedic exam, client videos of movement
|
Multimodal pain management; home modifications (ramps, rugs); weight loss programs; referral to veterinary rehabilitation specialists
|
MetLife and other providers cover alternative therapies like hydrotherapy and acupuncture, which are core to managing senior mobility issues.
|
[1], [2], [3]
|
|
Cognitive Dysfunction (CCD/FCD)
|
Senior / Geriatric Dogs and Cats
|
Lipoic acid, L-carnitine, high EPA/DHA, Antioxidants, Medium-chain triglycerides (MCTs)
|
DISHAA acronym, CADES (Canine Dementia Scale), MRI (rule out structural disease), Neurological exam
|
Environmental enrichment (puzzles, training); Selegiline (labeled drug); manage caregiver burden (sleep disturbances); Senior Care Kits
|
While behavioral medications are covered by many plans, the frequent follow-ups required for senior cognitive care benefit from plans with higher reimbursement rates.
|
[1], [2], [3]
|
|
Obesity and Weight Management
|
Middle-Aged to Senior Pets
|
High protein (spare lean mass), moderate to high fiber (satiety), L-carnitine, moisture (cats)
|
BCS > 5/9, morphometric measurements, daily BW checks (hospitalized), weighing food with gram scales
|
Limit treats to <10% daily calories; phone follow-up within 2 days of plan start; weigh-in appointments every 4-8 weeks; use of automatic feeders
|
Preventing obesity reduces premiums for long-term health by avoiding the development of comorbid conditions like diabetes and osteoarthritis.
|
[1], [4]
|
|
End-of-Life & Palliative Care
|
Senior Pets with Terminal/Chronic Disease
|
Palatable foods (resumption of favorites), appetite stimulants, enteral/parenteral feeding if indicated
|
Validated QOL assessments/scales, joy-of-living lists, pain scales
|
Initiate palliative care early; compassionate truth-telling; discuss euthanasia vs. palliated death; follow-up support for bereavement/grief
|
Embrace is noted for covering euthanasia and end-of-life expenses, including cremation and urns, through wellness rewards.
|
[2], [3]
|